If a plan does not appear in the Available Plans list, you can add a plan to a proposal manually by using the Add Plans feature. This functionality includes:
Plan Design: Enter information about the plan’s benefits structure. Dynamic costs: Enter age-banded and/or composite rate information; costs will update automatically based on changes to the employee census and employer contribution settings.
Supporting Documentation: Upload the plan summary or SBC, provider directory, and drug formulary to be linked on the proposal. You can also upload the carrier’s quote for your future reference.
Current and Renewal plans: Mark plans as the group’s current plan to customize a proposal to show their existing plan and renewal rates. Current plans are differentiated visually in the proposal.
Simple navigation: Plans you add to a proposal are found on the Plans Added tab on the Available Plans screen of each product line.
Edit Available Plans: Turn existing plans into a user-added plan with the click of a button to edit any of that plan’s information: rates, plan design, or documentation.
Employee elections: Manually added plans can now be included in an enrollment in Benefitter so that you can take advantage of Benefitter’s employee election functionality. Before you do so, please make sure that the carrier accepts a spreadsheet enrollment and that Benefitter’s elections spreadsheet includes all the data you’ll need to complete the carrier enrollment.
Add a Plan
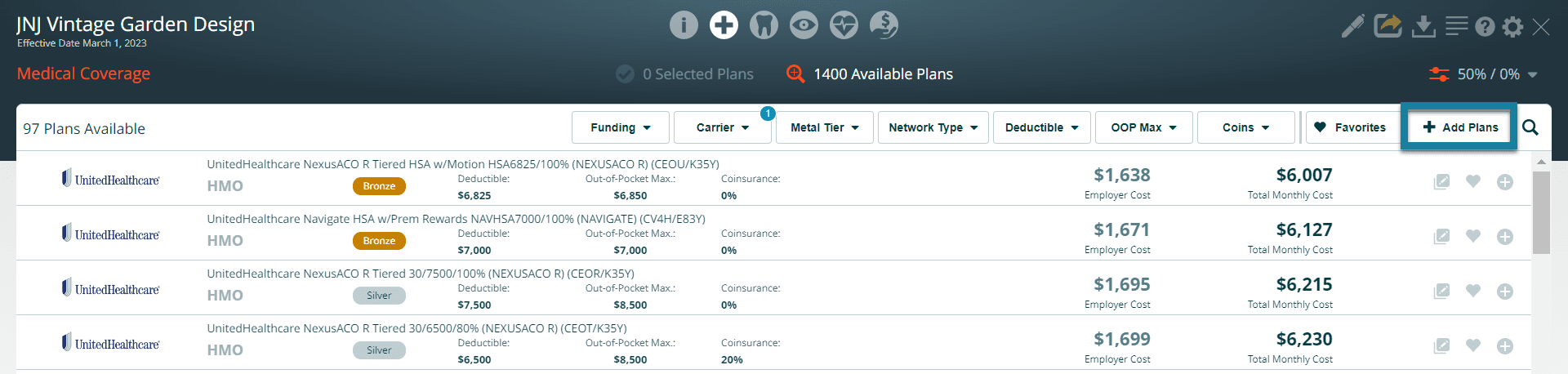
To add a user-added plan to the proposal, navigate to the Available Plans list of the appropriate coverage type (medical, dental, vision, life) in the proposal and click on the Add Plans button.
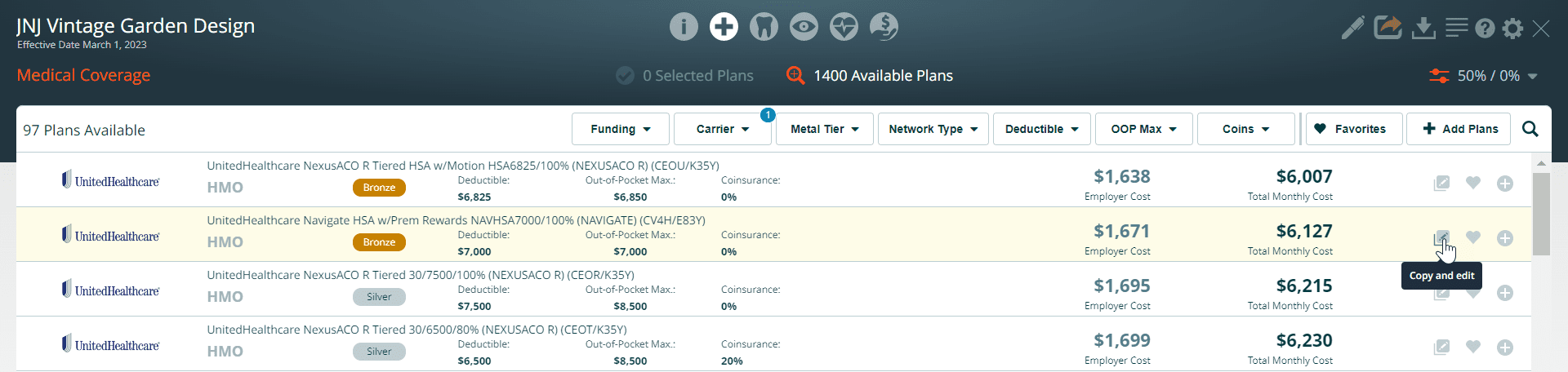
To turn an existing plan into a user-added plan, click on the copy and edit of a button to revise any of that plan’s information: rates, plan design, and documentation.
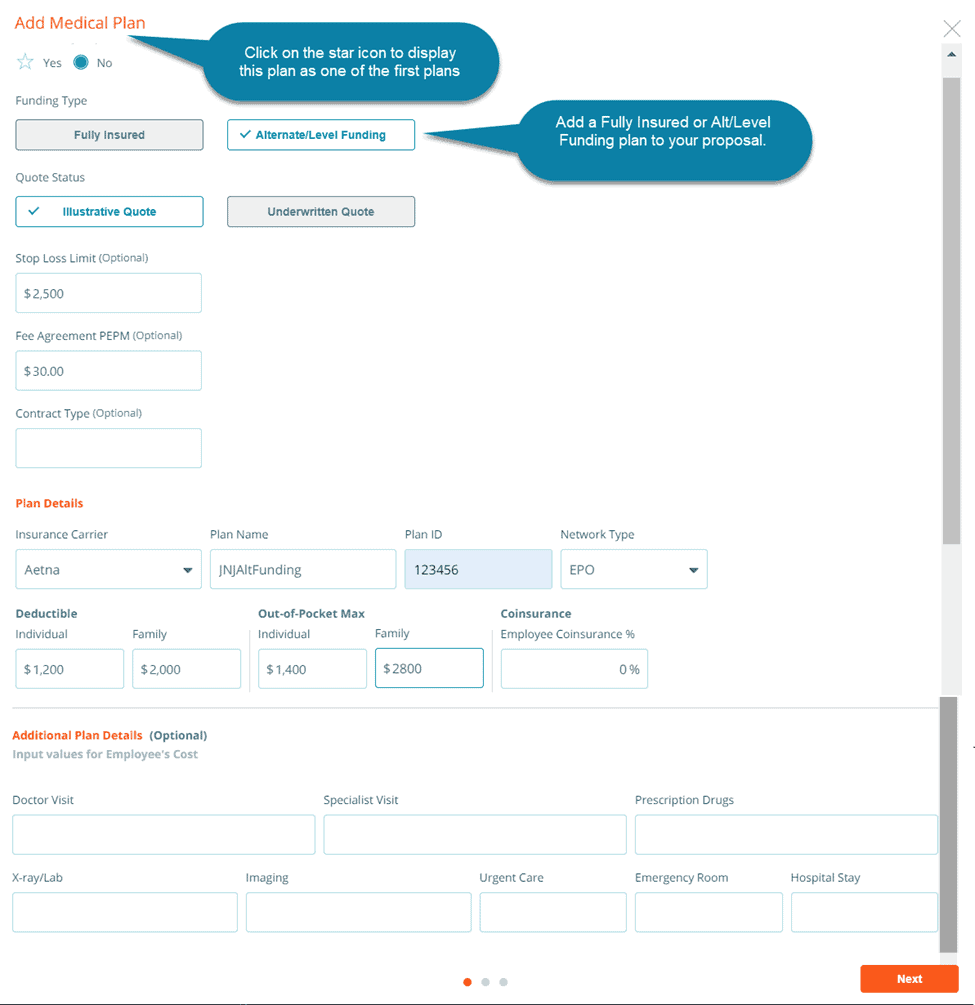
Plan Design
For all lines of coverage, you will begin by entering information about the plan design.
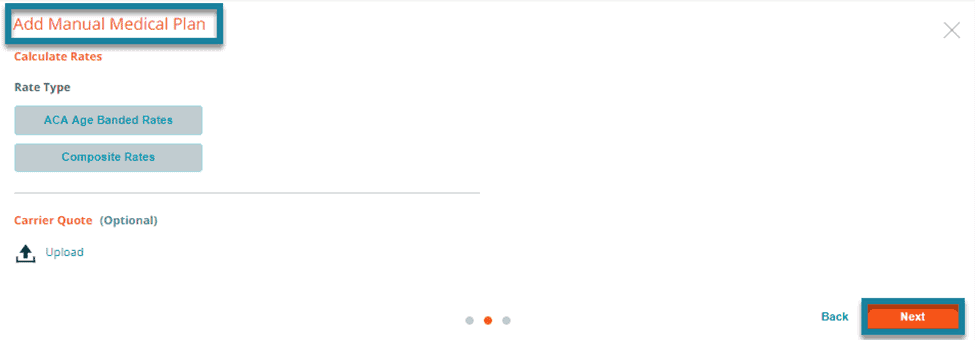
Rates
Composite Rates
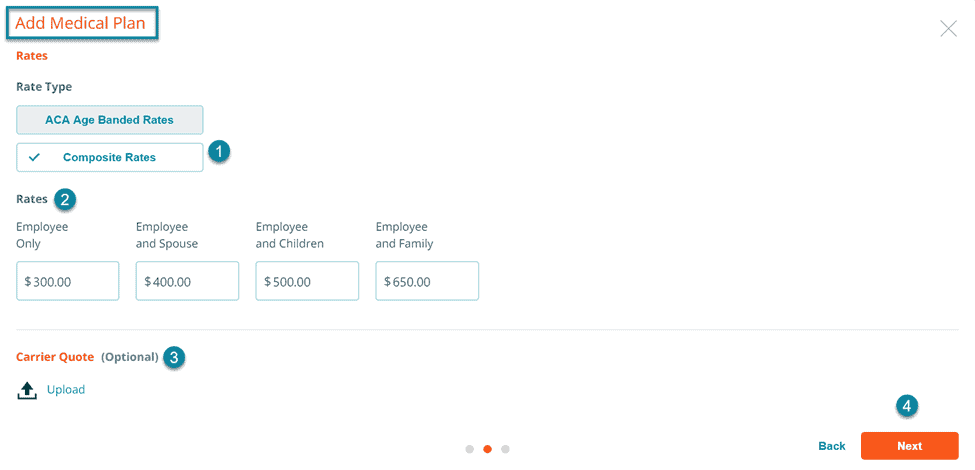
You can enter composite rates when adding a medical, dental, or vision plan. If you are adding a medical plan, you will be asked to select the Composite Rates option to reveal the fields for entering composite rates.
Enter the monthly composite rate for the Employee, Employee and Spouse, Employee and Children, Employee and Family and press the calculate button. We recommend that you upload a PDF of the carrier’s quote for your future reference.
ACA Age Banded Rates
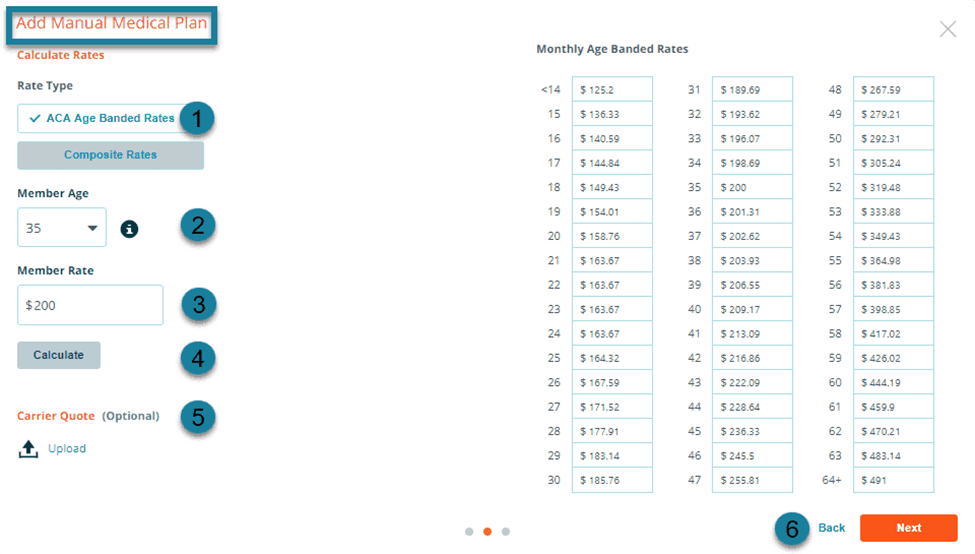
ACA Age Banded Rates Age-banded rates are available only for medical plans. It will calculate an age-table based on ACA rating rules from a single age rate that you enter. To generate the age-banded rate table, select the ACA Age Banded Rates button, choose age between 14-64, and enter the rate for that age in the Member Rate field. Click on the Calculate button to populate the monthly age-banded rates based on the state’s age curve. This table is editable. We recommend that you upload a PDF of the carrier’s quote for your future reference.
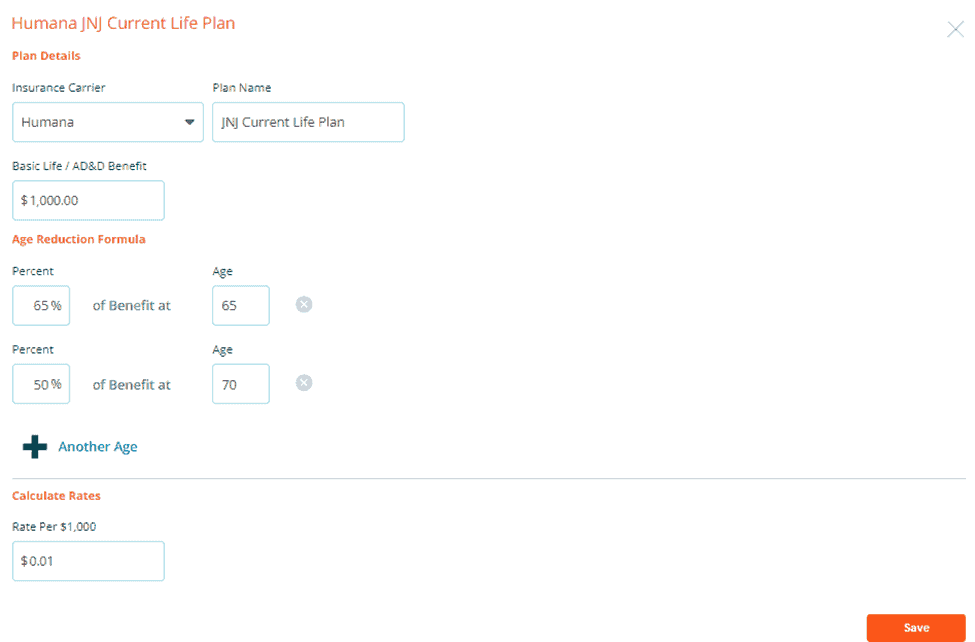
Rate per $1,000
Rates for user-added life plans are entered as the cost per $1,000 benefit.
Upload Plan Documents
When you add medical, dental, and vision plans, you have the option to upload the plan summary, provider directory, and drug formulary. These documents will appear on Selected Plans screen on the plan detail view. Enter the reason why you added the plan; we will monitor your feedback so we can continuously improve and update the system to resolve errors, assess demand for additional carriers, etc. Press the Save button to finish. You will now see the list of plans you have added to this proposal. Select a user-add plan for your proposal by clicking on the + icon in its row. To create additional plans, return to this screen (using the Plans Added button) and click on + Plan, found underneath the plans you have added.

Enter the reason why you added the plan; we will monitor your feedback so we can continuously improve and update the system to resolve errors, assess demand for additional carriers, etc. Click on the checkbox to delete carrier quote information. To add more user-added plans to your proposal, click on the plus icon.
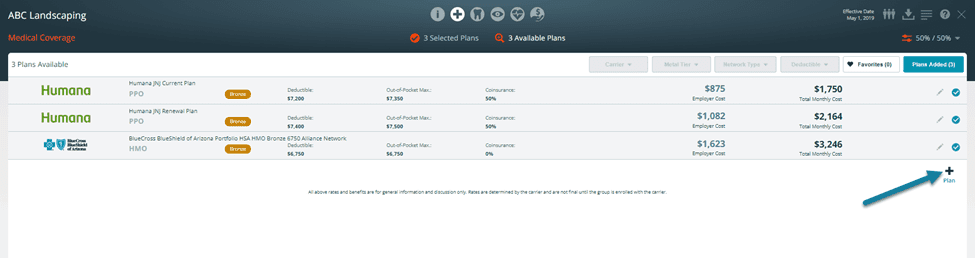
To edit your user-added plan, click on the pencil icon.
During the review process, if you make changes to the plan options press the save button. You can use the Back button to go to the previous page.

View User-Added Plans on your Proposal
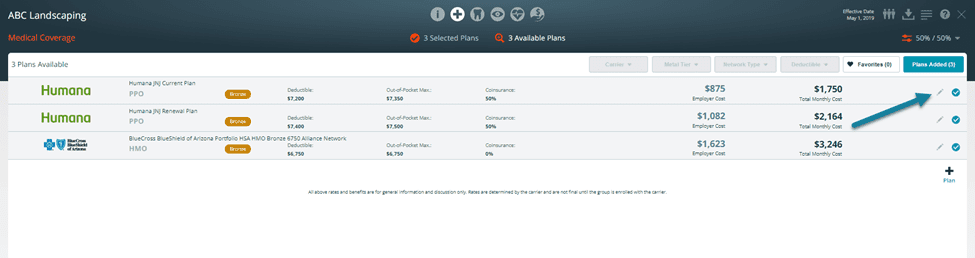
Your user-added plans will appear on the Selected Plans screen of your proposal alongside plans you select from the Available Plans screen. Plans that you mark as the group’s current plan are distinguished visually on the Selected Plans screen:
- Shown in shades of blue grey instead of teal
- Denoted by a star instead of a number
- Using this method you can provide your customers with a side-by-side comparison of the group’s current plan, renewal option, and new plans.
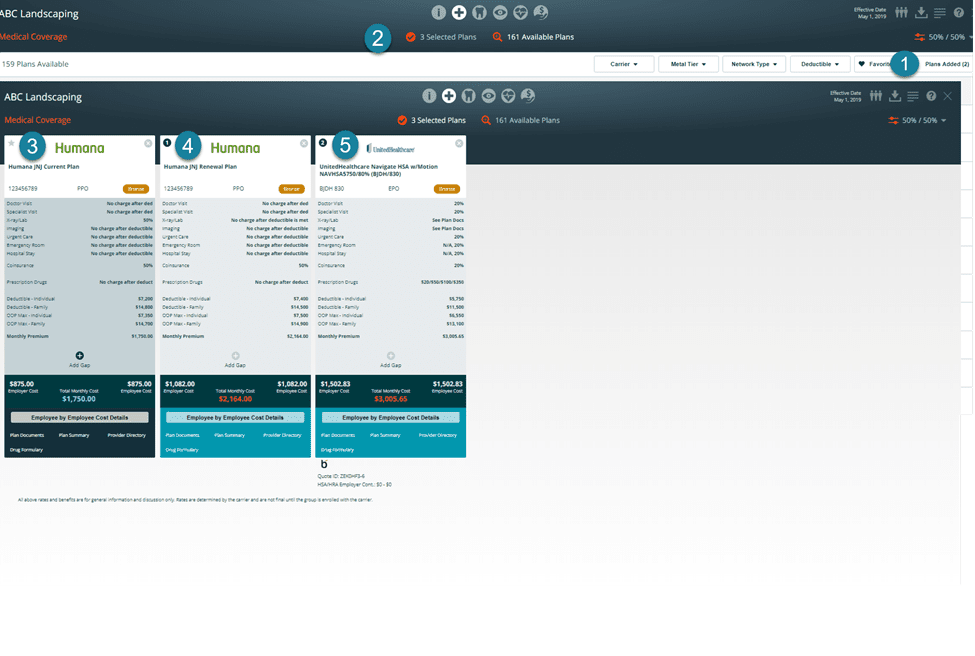
Include user-added plans in an Enrollment
You can include a user-added plan in an enrollment just like you would any other plan. This enables you to utilize Benefitter’s employee election functionality.
Please note that Benefitter is unable to confirm information for plans you add in the way it normally does. You will, therefore, be asked to verify the following during the enrollment setup process:
- Employee by employee cost details
- Confirm that the rates are correct before proceeding. If you find any errors, cancel out of the enrollment setup, modify the information in the proposal, and begin the enrollment setup again
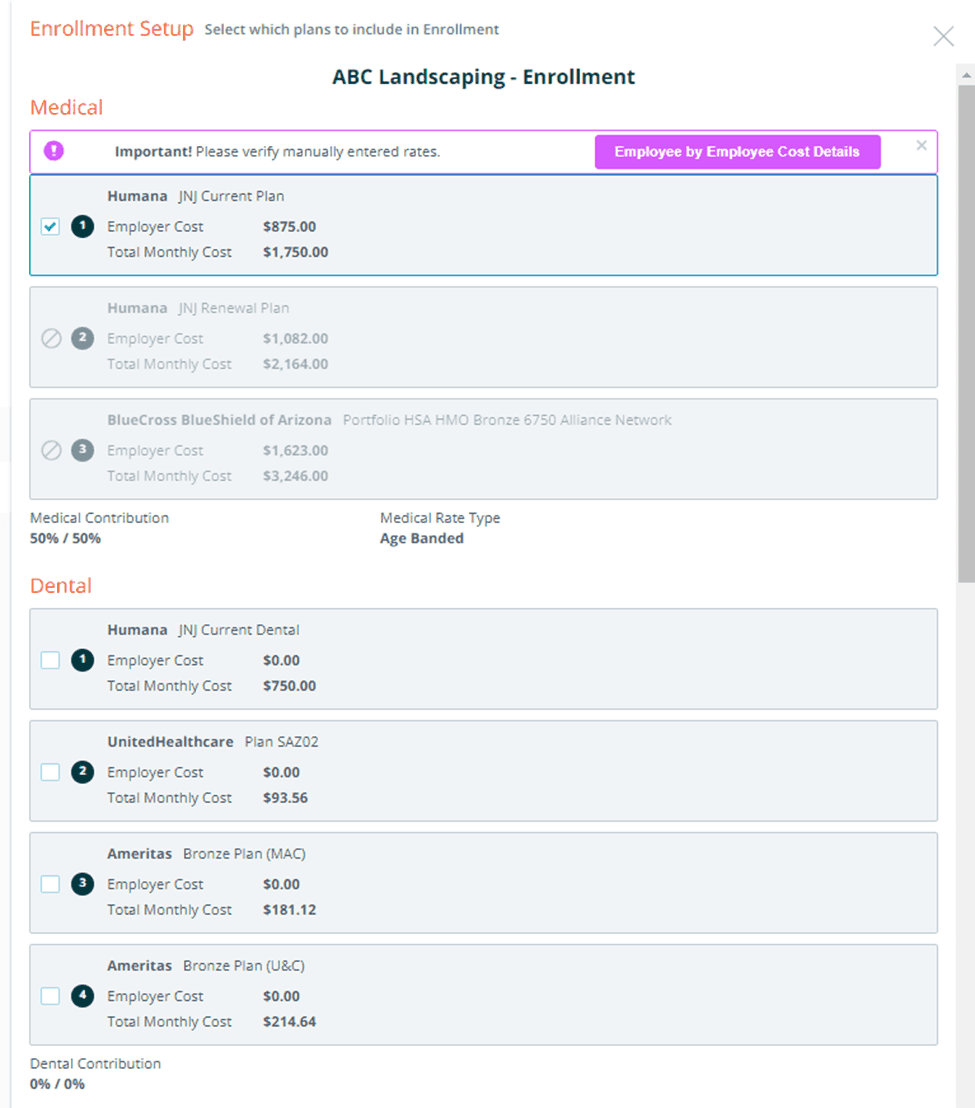
Carrier requirements for employee elections
Please ensure that you are familiar with the carrier’s requirements before using Benefitter for employee elections with a user-added plan. If the carrier accepts spreadsheets for employee elections, download Benefitter’s employee elections spreadsheet from the warning at the bottom of the enrollment setup screen and confirm that it contains all of the fields required. If the employee elections spreadsheet does not meet your needs, or if the carrier does not accept employee elections spreadsheets, please ask employees to fill out application forms instead.
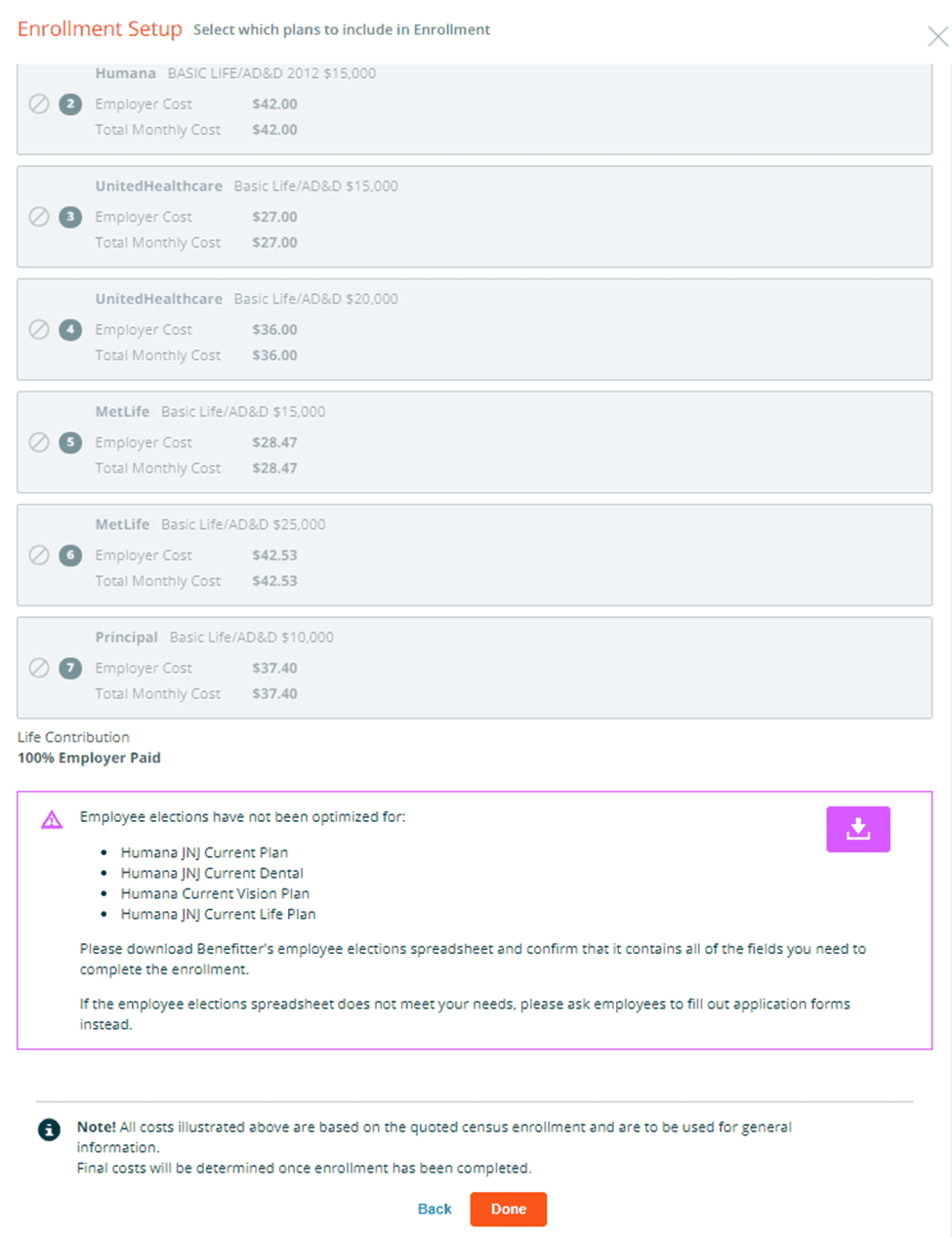
If you add a Humana manual plan, the enrollment will not be eligible for Humana eSubmission.
