Benefitter enables you to submit enrollments to Humana electronically—no paper required at any point in the enrollment process!
Which cases qualify for Humana e-Submission
- Combinations of Humana medical, PPO dental, vision, and/or life plans
- Groups located in Alabama, Arizona, Arkansas, California, Colorado, Connecticut, District of Columbia, Florida, Georgia, Idaho, Illinois, Indiana, Iowa, Kansas, Kentucky, Louisiana, Maine, Maryland, Michigan, Minnesota, Mississippi, Missouri, Nebraska, Nevada, New Jersey, New Mexico, New York, North Carolina, North Dakota, Ohio, Oklahoma, Pennsylvania, South Carolina, South Dakota, Tennessee, Texas, Vermont, Virginia, West Virginia, Wisconsin
- Plans that were manually added to Benefitter
- DHMO dental plans
- Groups located in Delaware, Hawaii, Montana, Oregon, Rhode Island, Washington
- Paper Submission only: Massachusetts, New Hampshire, Utah
Submission Overview
Notes:
- The group must be completely submitted (group number created and EGA signed) through Benefitter before the first of the month.
- If you have a group enrolling in Alt/Level Funded and Humana Specialty Plans, you will need to process the enrollment separately. You cannot use the Humana Electronic Submission feature. Refer to How to process an Alt/Level Funded & Humana Enrollment
The process of submitting a case electronically through Benefitter is divided into four stages:
1. Start Group Application. During this stage, Benefitter collects the information you would normally provide on the group application form:
- company information.
- Eligibility rules
- Prior dental and ortho coverage (if applicable).
- Agent of record and writing agent
- Payment information
- Client signature Writing agent signature
The employee enrollment elections must be completed before you can start this process.
2. Review Elections This is your final opportunity to review employees’ benefit elections and enrollment information for completeness and accuracy. Final updates can be made at this time.
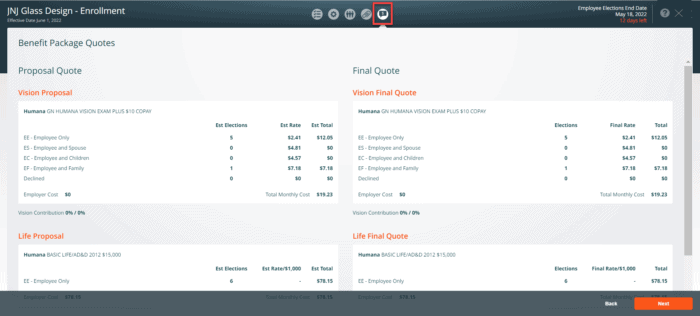
3. Confirm Final Quote and Submit This screen compares the Proposal Quote and Final Quote, giving you and the client a chance to see how enrollments and costs have changed from what was predicted for the proposal.
4. Confirmation The confirmation page notifies you of any errors in the submission and, upon successful processing of the case by Humana, provides the group ID (usually within a few hours of submission).
5. Humana eElectronic Submission Status Indicators Notifications As you progress through the stages of the Humana Electronic Submission process, Benefitter displays status indicators on the agent and company homepages.
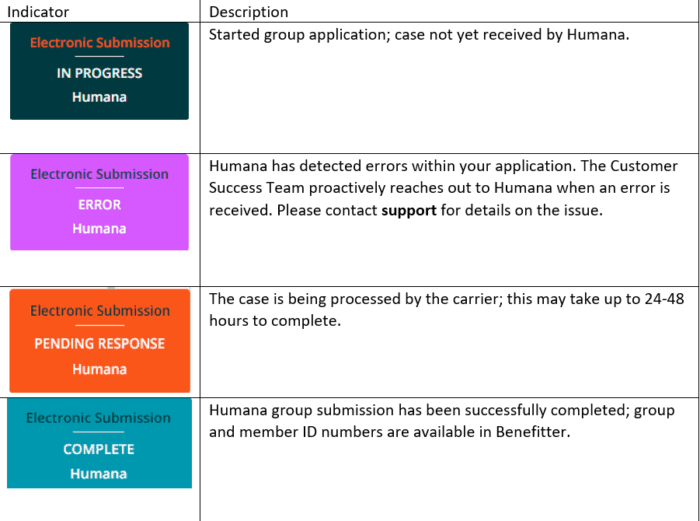
Below you will find a chart of the indicators and their definitions.

Start Enrollment and Group Application
All employee elections must be completed before you can initiate the Humana electronic submission.
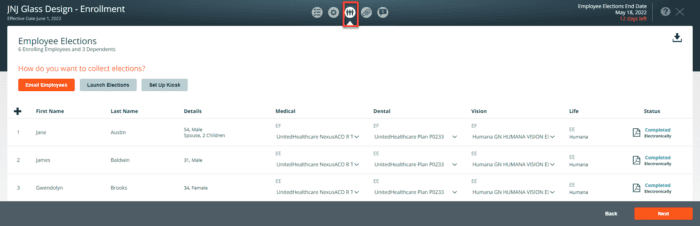
To initiate the Humana electronic submission, click on the Carrier Enrollment (paper clip icon). Press the start button to process the paperless enrollment. The Carrier Enrollments screen shows the enrollment options for all carriers included in the enrollment. All employee elections must be completed before you can initiate the Humana electronic submission.
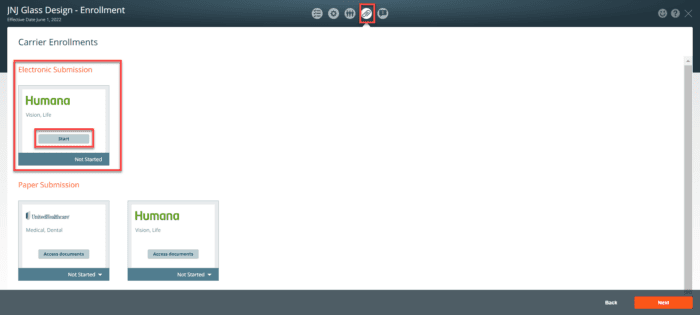
Note: This feature is available only to new business groups; groups with existing Humana coverage are not eligible. For the business to qualify for small group medical coverage, it must meet one of the following conditions:
- A) The business is a partnership with at least one employee enrolling in the medical coverage, or
- B) The business is wholly-owned by one person and has at least one employee who is not the owner or the spouse of the owner enrolling in the medical coverage.
Group Application
This stage collects the information you would normally provide on the group application form. Much of this information is already filled out based on the information in the company profile and proposal. Unless otherwise specified, the fields in the Start Group Application stage are required. Confirm that information is accurate and complete the few additional fields, which include established date, type of business, and tax ID/EIN.
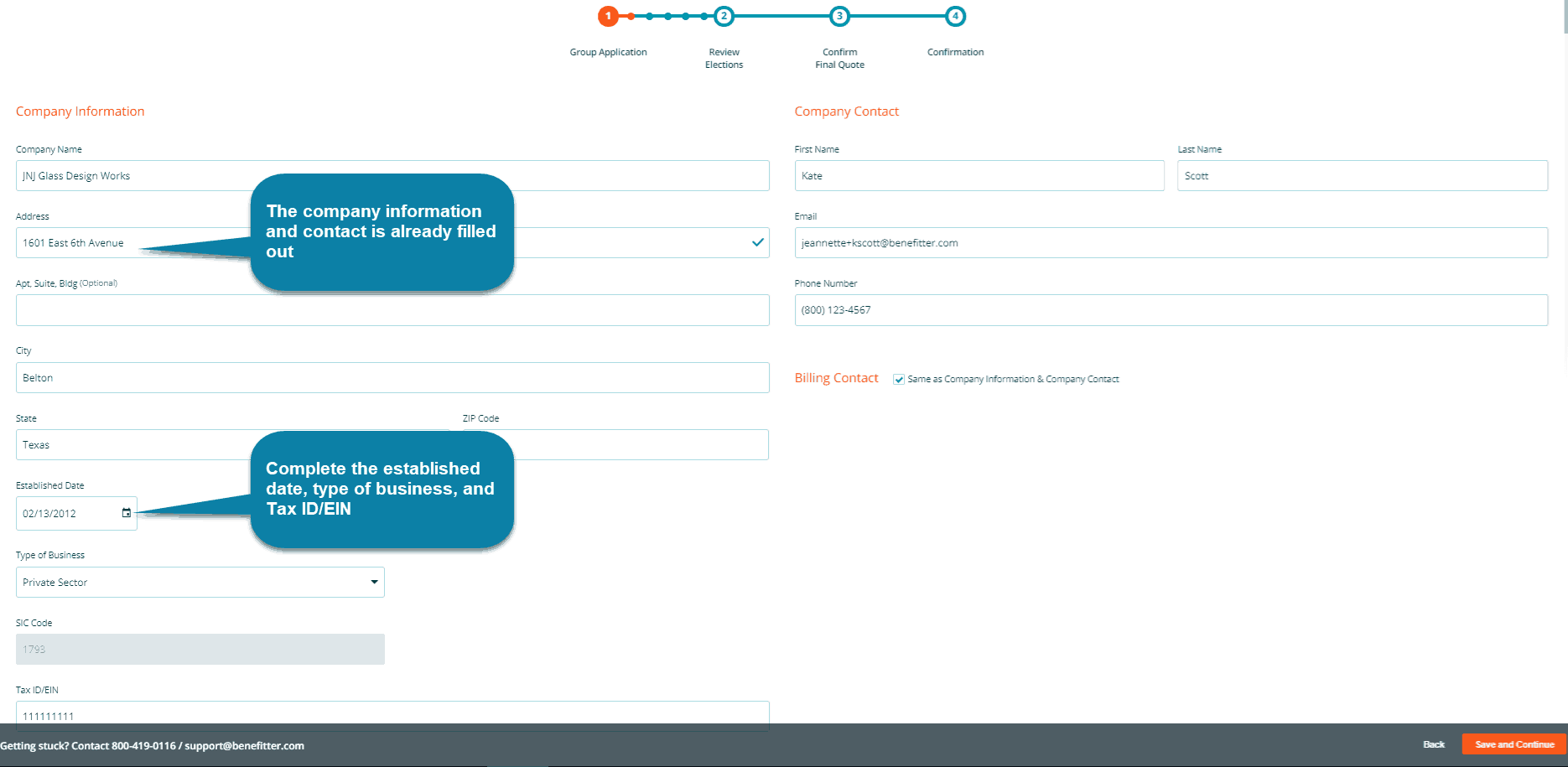
Benefitter uses USPS to validate addresses. If you’re having trouble with the company address on this screen, please verify whether the address is valid by entering the street address, city, and state into USPS’s Zip Code Lookup Tool and work with the employer to determine a valid address for their company. Clicking on Save and Continue brings you to a page where you’ll fill in the client’s waiting period, as well as information on any prior dental coverage. If you select yes for prior dental coverage, you will be asked to enter the insurance company and termination date.
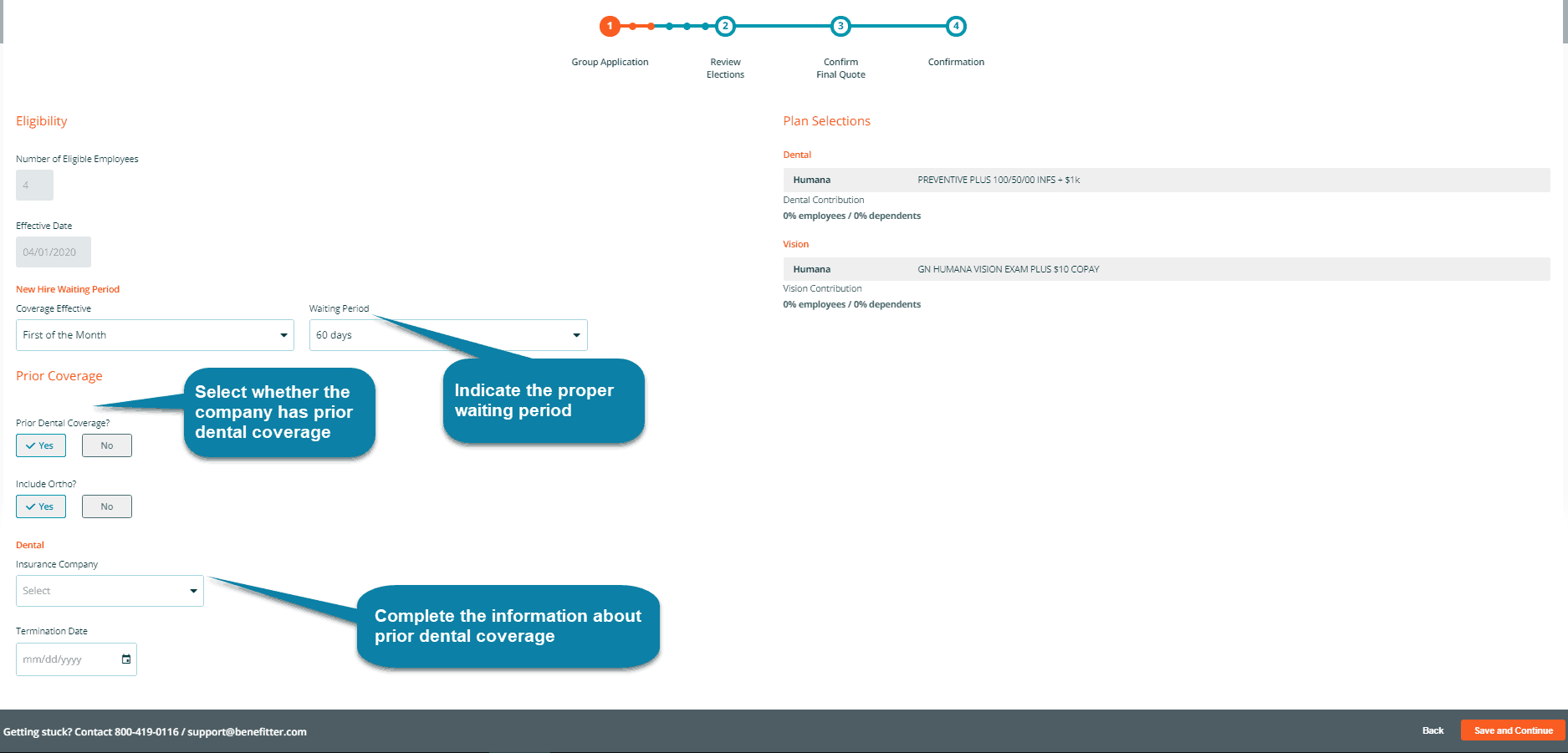
The next page requests information about the agents and agencies involved in the case, including the Tax ID/EIN that Humana has in their systems. You can have 1–2 agents of record and 1–2 writing agents. Begin by indicating whether the Agent of Record is an agency, then fill out the requested information.
If you have more than one agent involved in the case, you can adjust the commissions split between them.
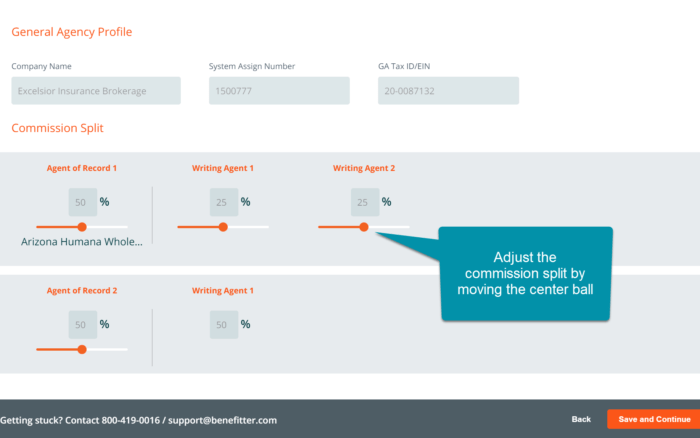
The sum of the writing agents’ percentages and the sum of the agent of records’ percentages each equals 100% (i.e., all agents’ percentages are represented as a percent of the total commission). Make sure to designate the writing agents’ commissions as coming out of the correct AORs’ commissions.

To submit the group application, click on the ‘Submit Group Application to Humana’ button.
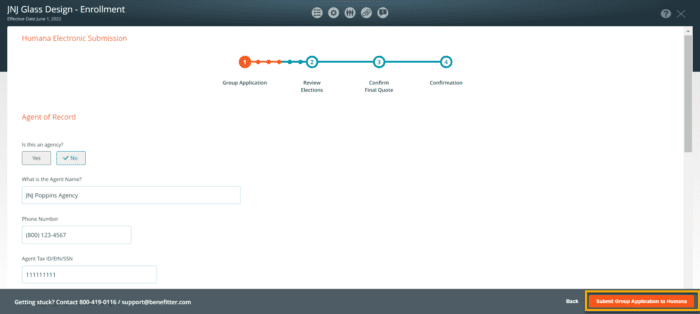
After the group application has been submitted, it takes a few minutes to complete. Click on the X icon to exit out of the page.
The group id will be populated on the page.
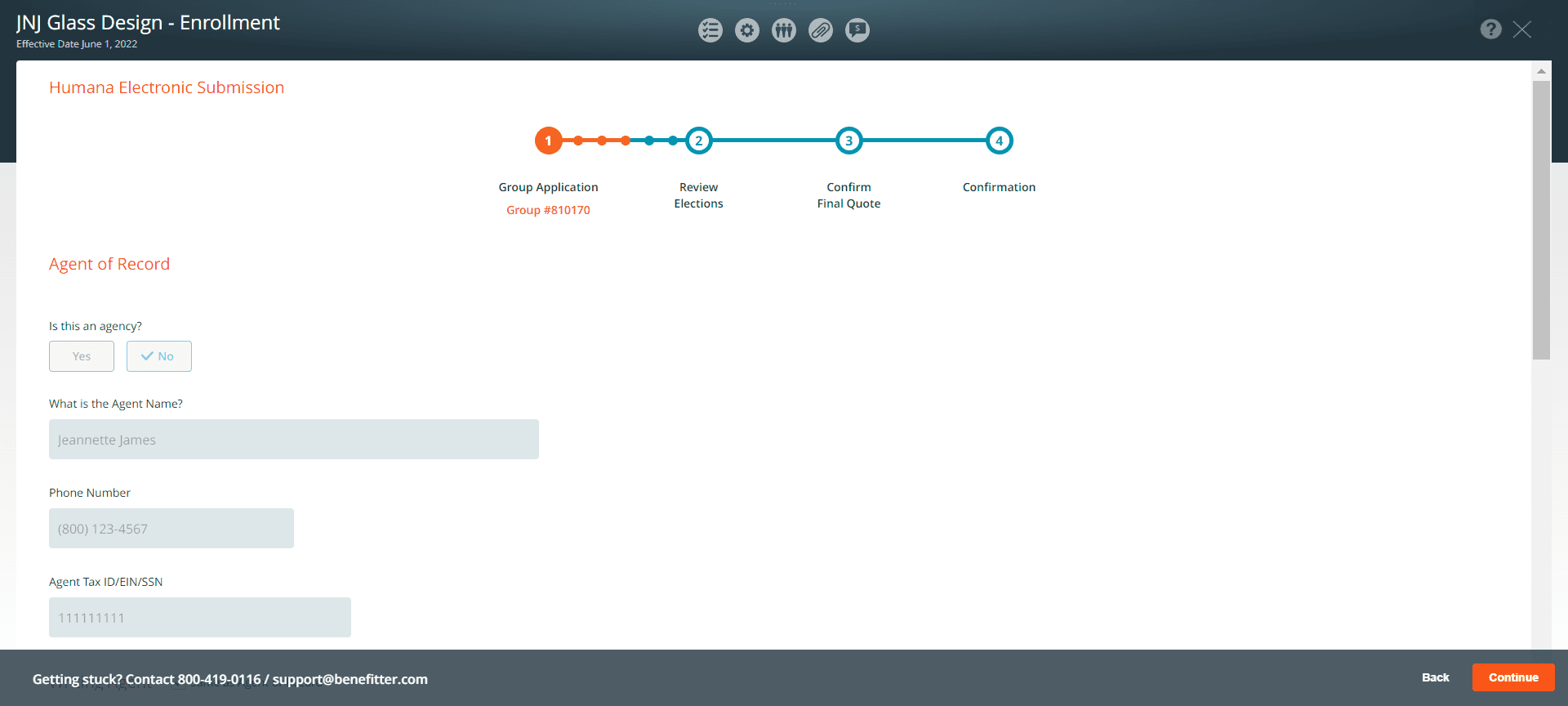
Collect Employer Signature
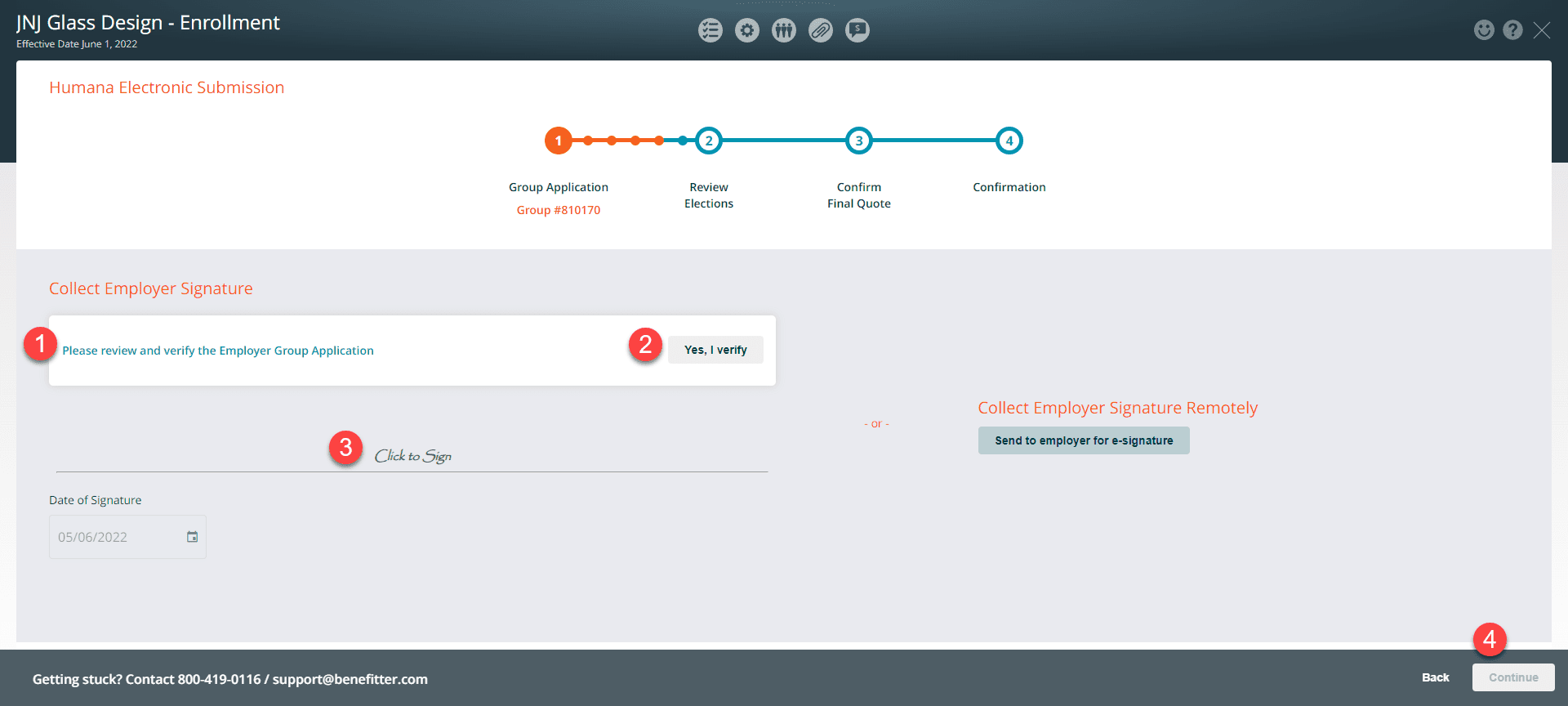
You can collect the employer’s signature in person, or send an email to collect an e-signature remotely. The employer needs to review the Employee Group Application and sign/verify the application.
In Person – to collect the signature the employer needs to:
- Click on the ‘Please review and verify the Employer Group Application’ and review the Employer Group Application
- Click on the ‘Yes, I Verify’ button
- Sign the Group Application
- Press the continue button
Employer Group Application
Employer enters their first and last name
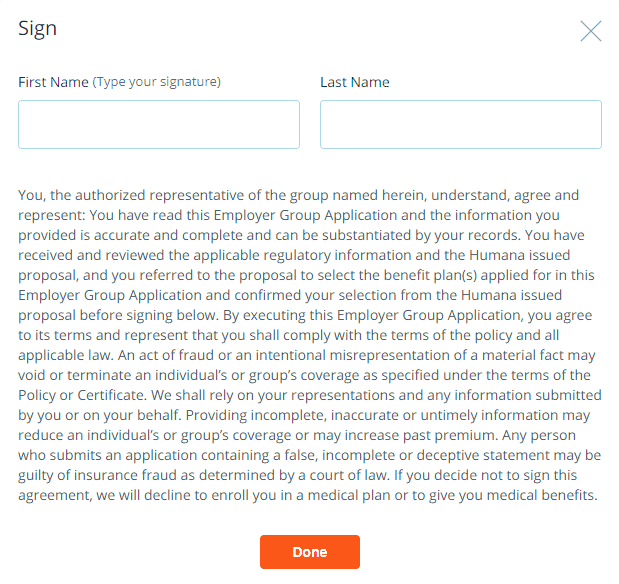
The Employer’s signature will be populated on the Group Application
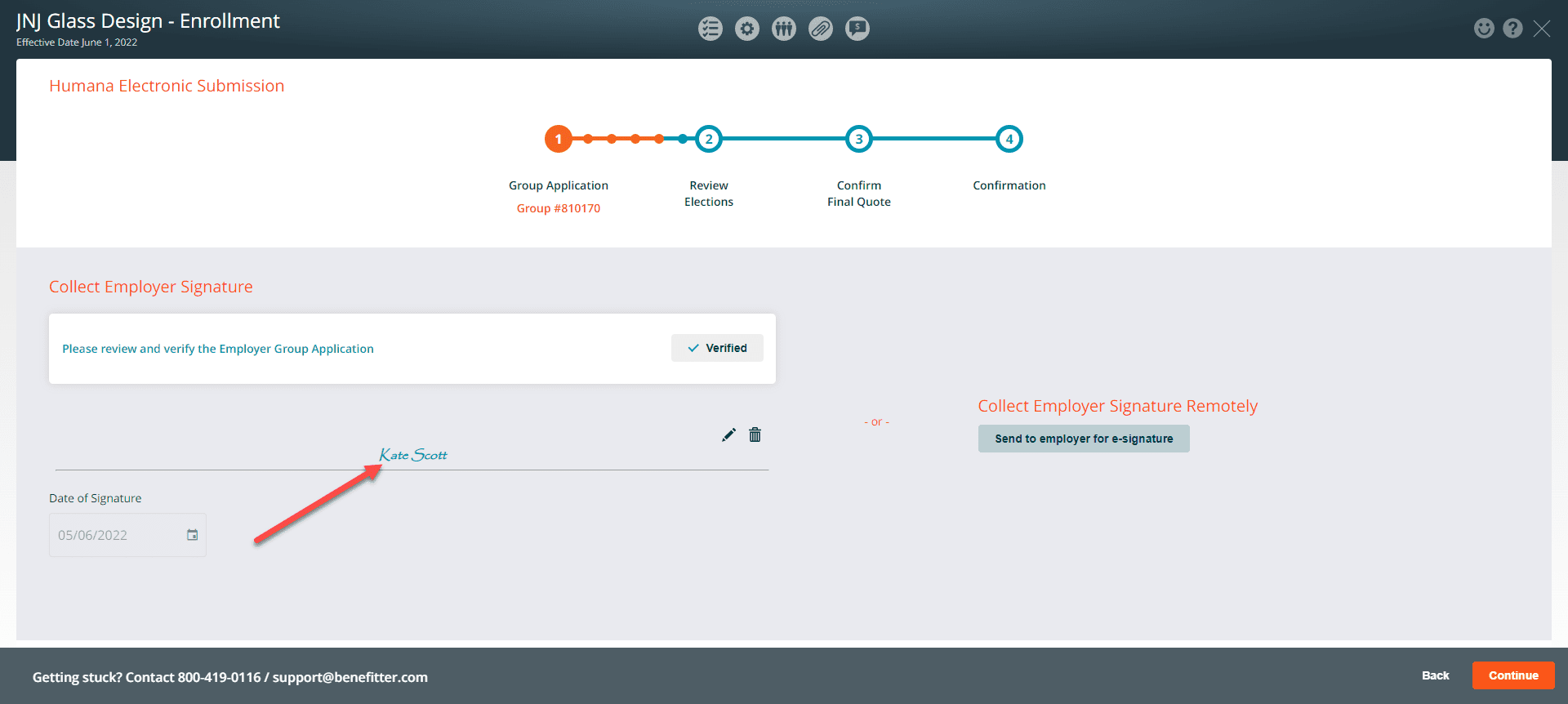
Collect the Employer signature remotely
Click on the ‘Send to employer for e-signature’ link.

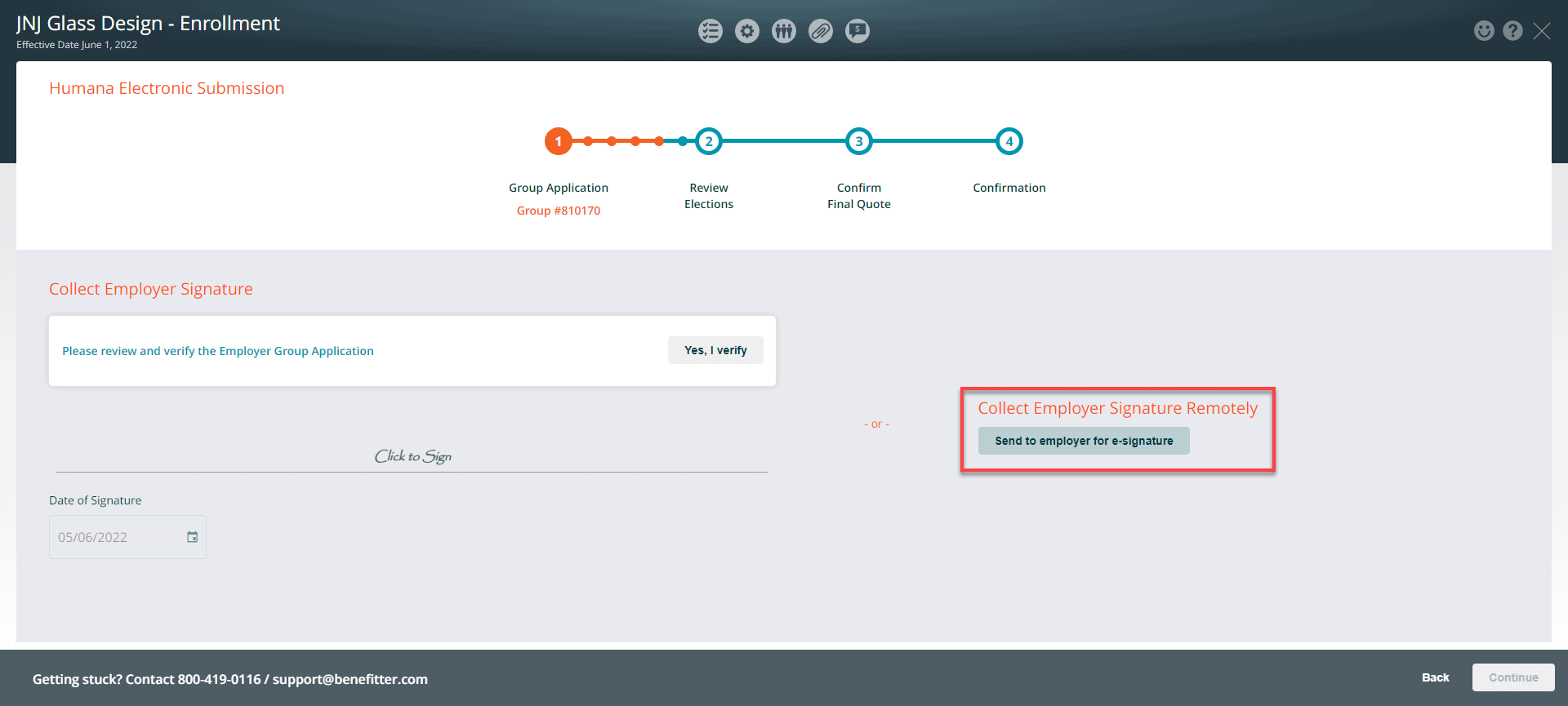
Click on the send button to forward the email to the Employer.
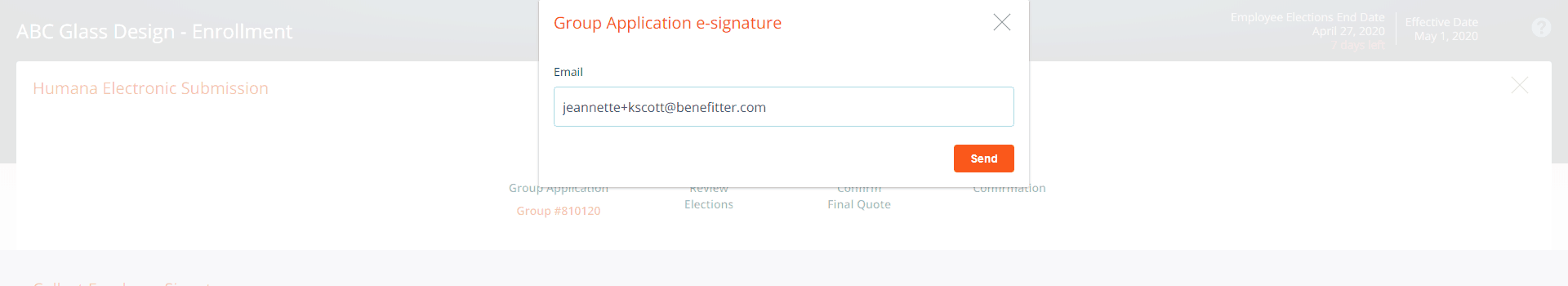
The employer will need to click on the email with the Subject Line ‘Action Required: e-signature for Humana insurance application’. In the body of the email the employer needs to click on the ‘Sign Now’ button.
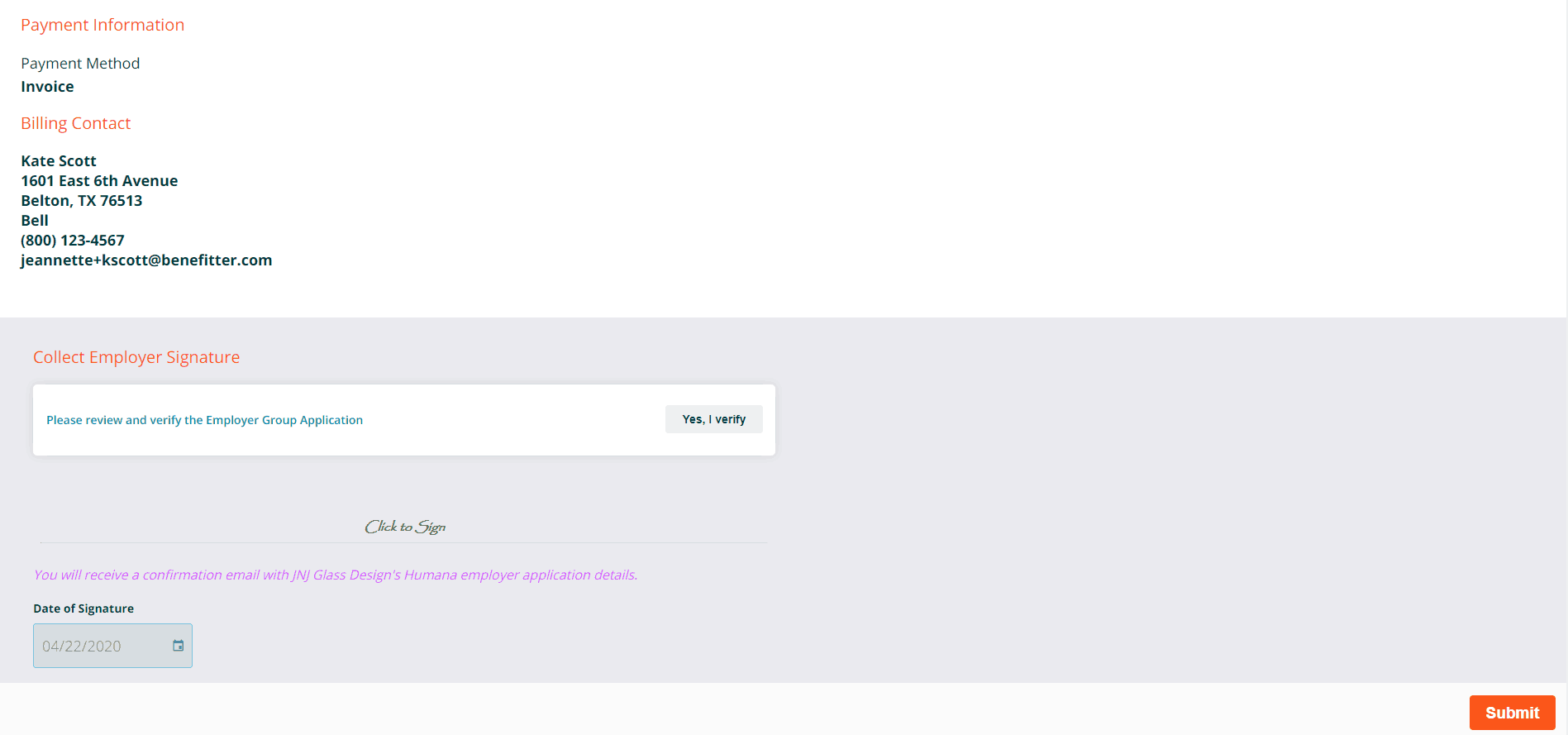
On the remote e-signature page, the Employer must review the details on the Humana group insurance application carefully. Complete the signature form at the bottom of the page. If there are any inaccuracies, the Employer needs to contact the agent to have the information corrected.
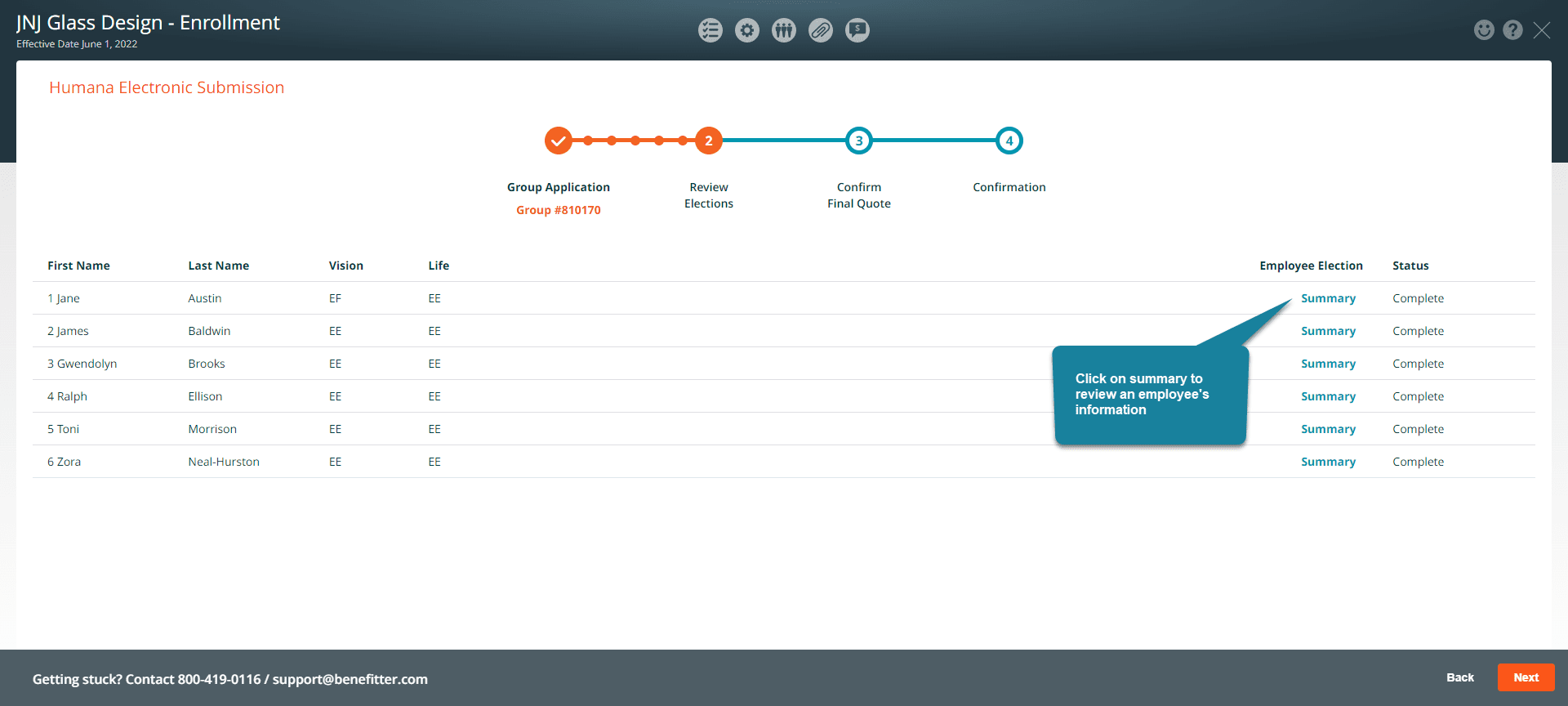
Review Elections
The Review Elections screen shows you the status of the employees’ benefit elections. Any incomplete elections or errors are called out on this page. Please confirm that all elections are accurate before proceeding.
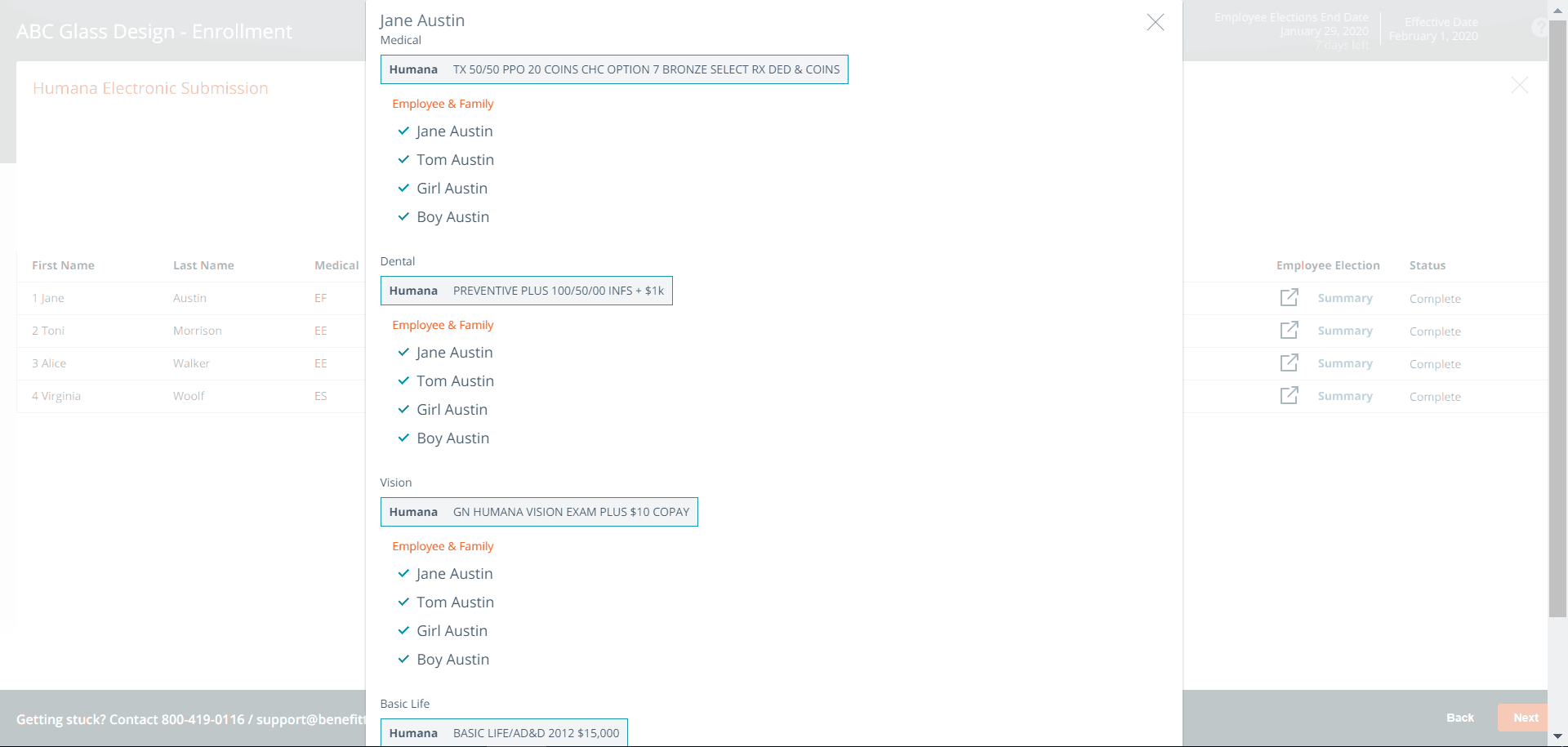
Employee Election Summary
Confirm Final Quote
This screen compares the Proposal Quote and Final Quote side by side; changes are shown in red. Click on the Submit to Humana button at the bottom of the Confirm Final Quote screen. Please do not press this button unless the case is final and ready to be submitted to Humana, and do not submit any test cases.
Enrollment Confirmation
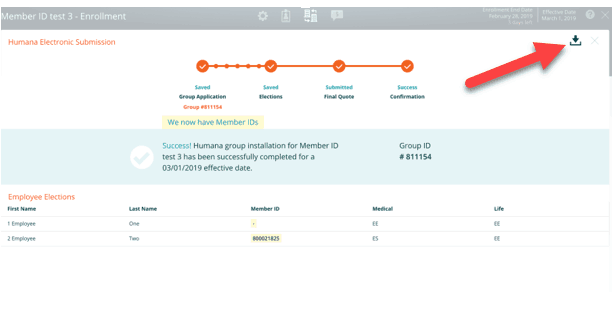
Group ID, Member IDs, and Employer Group Application
The confirmation screen displays the status of your submission, including any errors that would require you to edit and resubmit the case. The group ID number is usually available within a few minutes, while member IDs are usually available within 48–72 hours. Once the member IDs are populated on the Humana Electronic Submission page, you can download the spreadsheet that contains the group and member IDs to send to the Employer. The Employer Group Application can also be downloaded and sent to the Employer. The group and member IDs are also displayed on the Employee Election page. You will receive an email letting you know that the member ids have been populated on the system.
The Benefitter Support Team proactively monitors eSubmission enrollments and will contact you to review any issues with the enrollment. If there is an issue with the enrollment please do not resubmit the enrollment. To contact Benefitter Support for assistance, call (800) 419-0116 or send an email to support@benefitter.com; include the group’s name and effective date in the email body.
Welcome Letter and Post Submission Changes
You will receive the official welcome letter as an email from the customer success team within a few days of the group number being finalized. Once a submission has been received and accepted by Humana, no changes can be made to the submission (either group information or employee details) through Benefitter. Please use Humana’s existing book of business tools to make corrections and add/change/deletes.
Troubleshooting Tips:
- Enter all the required fields on the company information page prior to creating a proposal. This way, you don’t have to go back to the client to ask for data such as tax information. To save time, obtain the company’s Established Date it is a required field on the Group Enrollment Application.
- Employee mailing addresses cannot be a PO Box address. If you’re having trouble with the company address or employer mailing address on the Humana Submission screen, please verify whether the address is valid by entering the street address, city, and state into USPS’s Zip Code Lookup Tool and work with the employer to determine a valid address for the company and employee and update the address and resubmit the enrollment.
Next: Paper Submission
